Traveling from Woodbridge for Dental Implants: What to Expect at Your First Visit
A first implant visit in Maple is a planning appointment, not a treatment session. Expect a full clinical review, 3D imaging where needed, and a step-by-step plan that covers suitability, preparation, timing, and costs. Patients travelling from Woodbridge usually leave with a clear, written outline of what will (and will not) be done, and why.
Table of Contents
- Why patients come from Woodbridge to Maple
- What to sort out before you go
- How the first visit is structured
- Imaging and what it actually shows
- Building a treatment plan that holds up
- Timeframes: what is typical and what is not
- Cost structure without guesswork
- Getting from Woodbridge to Maple
- Suitability: who proceeds and who needs preparation
- Comparison: quick check vs implant consultation
- Common assumptions that don’t hold
- Practical checklist
- Extended FAQ
- Sources
Why patients come from Woodbridge to Maple
The drive from Woodbridge to Maple is short. The reason people make it is not distance — it is the expectation of a more thorough assessment.
Implants are not decided on a quick look. They depend on bone condition, bite forces, and long-term stability. A careful first visit reduces later changes. That tends to matter more than proximity.
There is also a practical point. When planning is done properly at the start, fewer adjustments are needed later. That saves time overall, even if the initial visit takes longer.
What to sort out before you go
A first visit works better when basic information is available.
Bring:
- Recent dental X-rays if you have them
- A list of medications
- Notes on previous extractions or failed treatments
- Any known medical conditions
If nothing is available, that is not a problem. It simply means more will be done on-site.
Keep expectations neutral. Many patients arrive convinced they either “definitely need implants” or “probably cannot have them.” Both assumptions are often wrong.
How the first visit is structured
The appointment is usually organised in stages. It does not feel rushed when done properly.
Initial review
A short conversation about your history and current concern. This sets the direction of the visit.
Clinical examination
The dentist checks gum condition, spacing, bite, and how neighbouring teeth behave under load. This part often reveals issues patients are not aware of.
Medical context
Healing capacity matters. Smoking, diabetes, certain medications — these are not minor details in implant planning.
Focused discussion
Rather than general advice, the discussion moves toward your specific case: what is possible, what is not advisable, and what requires preparation.
Clinicians such as Dr. Carly Gordon typically approaches this stage by mapping out long-term function first, then working backwards to the surgical steps.
Imaging and what it actually shows
Most implant consultations involve CBCT imaging. It is not just “a better X-ray.” It changes the level of detail available.
A 3D scan shows:
- Exact bone thickness
- Hidden defects or voids
- Position of nerves
- Sinus boundaries in upper jaw cases
This matters because implants are placed in bone, not in teeth. Bone cannot be judged accurately from standard images.
Guidance from the Canadian Dental Association and the American Academy of Implant Dentistry supports 3D planning as a way to reduce placement errors and avoid avoidable complications.
Building a treatment plan that holds up
Once imaging and examination are complete, the dentist builds a plan. This is where many consultations differ in quality.
A proper plan answers:
- Is an implant the right option here
- How many implants are needed
- Whether bone grafting is required
- What type of restoration will be used
- How forces will be distributed
There is usually a clear sequence. For example, a missing molar with reduced bone may require grafting first, then placement months later. Trying to shorten that sequence can compromise stability.
Patients often notice that the conversation becomes more specific at this stage. Vague phrases are replaced with concrete steps.
Timeframes: what is typical and what is not
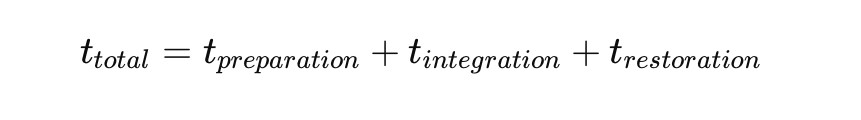
Implant timelines are not fixed, but they follow a pattern.
| Phase | What happens | Usual range |
|---|---|---|
| Consultation | Assessment and scans | 1 visit |
| Preparation | Extraction or graft if needed | 1–3 months |
| Placement | Implant inserted | Single visit |
| Integration | Bone fuses with implant | 3–6 months |
| Restoration | Crown or bridge fitted | 2–4 weeks |
What is often misunderstood: the longest part is not the procedure — it is the healing phase. That is where stability is gained.
Cost structure without guesswork
Costs are usually presented in parts, not as a single figure.
Typical breakdown:
- Surgical placement
- Restoration (crown, bridge)
- Additional procedures if required
This structure is deliberate. It allows patients to see where complexity affects cost.
A clear consultation should provide:
- A written estimate
- Explanation of optional vs necessary steps
- Clarification of what is included and what is not
Getting from Woodbridge to Maple
The route from Woodbridge to Maple is straightforward, usually under half an hour.
Practical considerations:
- Avoid peak traffic if possible
- Leave buffer time for the first visit
- For future procedures, consider whether you will need someone to drive you home
Distance rarely affects treatment quality, but planning around it avoids unnecessary stress.
Suitability: who proceeds and who needs preparation
Implants are not a default solution. Suitability depends on several factors.
Key considerations:
- Bone volume and density
- Gum health
- Smoking status
- Systemic conditions
- Previous dental history
In many cases, patients are suitable but not immediately ready. Preparation improves outcomes. That may mean waiting before placement.
Comparison: quick check vs implant consultation
| Feature | Routine dental visit | Implant consultation |
|---|---|---|
| Imaging | Basic X-ray | 3D CBCT |
| Time spent | 10–20 minutes | 30–60+ minutes |
| Outcome | General advice | Detailed plan |
| Cost clarity | Rough estimate | Structured breakdown |
| Risk assessment | Limited | Case-specific |
Common assumptions that don’t hold
| Assumption | What actually happens |
|---|---|
| Implants are done at the first visit | The first visit is diagnostic |
| If it doesn’t hurt, everything is fine | Bone issues are often silent |
| All cases are similar | Each plan is individual |
| Faster is better | Healing time is essential |
Practical checklist
- Bring any previous records
- List medications clearly
- Prepare specific questions
- Allow enough time for the visit
- Avoid scheduling immediately after
Extended FAQ
What is the main outcome of the first visit?
You should leave with a structured plan. That includes whether implants are appropriate, what preparation is needed, how long the process will take, and how costs are organised. If this is not clear, the consultation has not done its job.
Why is the first visit not used for treatment?
Implants depend on bone conditions that cannot be judged without proper imaging and planning. Placing an implant without that information increases the risk of failure or complications. The first visit is used to reduce those risks.
How accurate are the timelines given at the consultation?
They are estimates based on typical healing patterns. The actual timeline may shift depending on how your body responds, especially during the integration phase. The structure of the timeline, however, usually remains the same.
What if I am told I need bone grafting?
This is common. Bone changes after tooth loss, and grafting restores volume where needed. It is not a complication — it is often part of standard preparation for stable implant placement.
Is the consultation enough to decide whether to proceed?
For many patients, yes. The combination of examination and 3D imaging provides enough information to make an informed decision. Some patients may take additional time to consider options.
How detailed should the cost explanation be?
It should be broken into stages, with clear distinctions between necessary and optional procedures. A single combined figure without explanation is not particularly useful.
Does travelling from Woodbridge affect follow-up care?
Not significantly. Follow-up visits are spaced out, and the travel distance is short. Planning ahead for key appointments is usually enough.
Are alternatives discussed, or only implants?
Alternatives should be part of the conversation. Bridges, removable options, and doing nothing temporarily are all valid considerations depending on the situation.
What are the most common concerns patients raise?
Patients usually ask about pain, duration, and cost. Less often, they ask about long-term maintenance, which is equally important. Implants require ongoing care, similar to natural teeth.
How do I know if the consultation was thorough?
A thorough consultation leaves little uncertainty. You should understand the sequence, the risks, the timeline, and the cost structure. If answers feel vague, it is reasonable to ask for clarification.
Sources
- Canadian Dental Association — Patient guidance on dental implants, oral health standards, and clinical expectations in Canada
https://www.cda-adc.ca - American Academy of Implant Dentistry — Evidence-based information on implant procedures, planning, and outcomes
https://www.aaid-implant.org - National Institute of Dental and Craniofacial Research — Research-based information on tooth loss, bone health, and dental restoration
https://www.nidcr.nih.gov




















